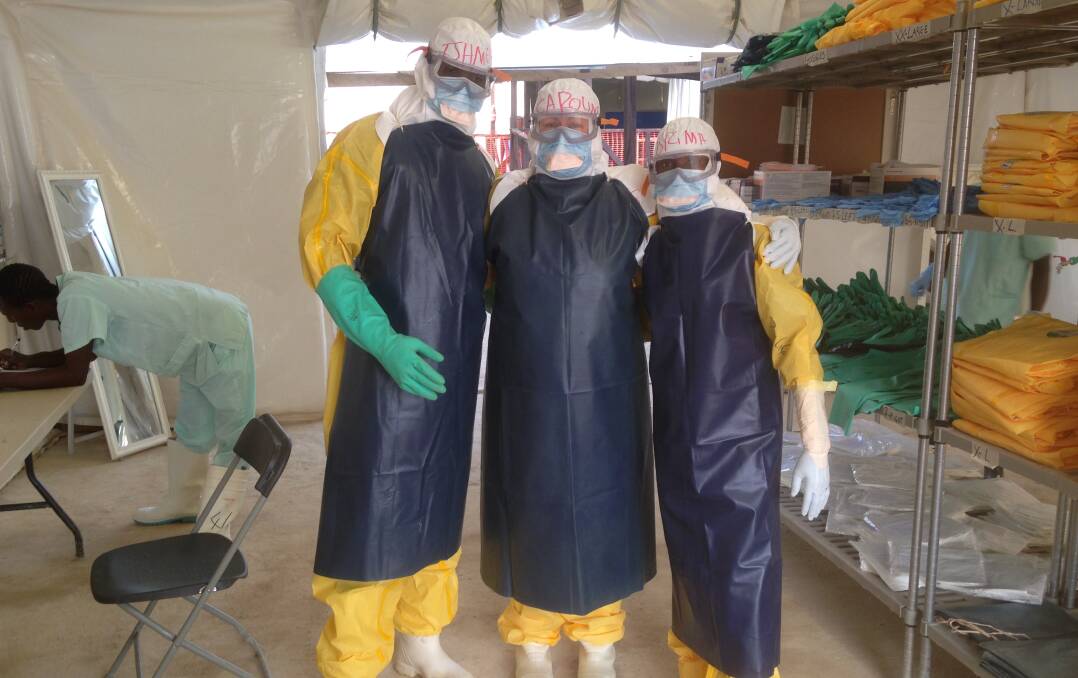
BALLARAT nurse Caroline Nash expected a six-week stint in a Sierra Leone ebola treatment centre to be a challenging medical experience.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
But luckily she was also aware it would be emotionally confronting.
"I was particularly moved when two siblings who survived the ebola virus were discharged," Ms Nash said.
"While this was a happy occasion, I felt mixed emotions as these children were now orphans, as both parents had died from the disease."
Ms Nash said patients who left the treatment centre were sent home with a letter certifying them as ebola-free.
"This reduces the likelihood of them being ostracised by family, friends and the community.
"For the ebola survivors, national staff sing the Ebola Go song (as they leave). It is an emotional time for everyone."
Ms Nash, who has a Masters in Public Health, volunteered for the Aspen Medical stint due to her love of travel and an interest in worldwide health patterns.
"I come from a big family of travellers and I'm very interested in global issues and international health."
Ms Nash arrived in Sierra Leone on February 22, with six other Australia and New Zealand health professionals.
Expatriate nurses, working in pairs, led five teams of local medical staff around the clock in the Hastings treatment centre, an hour from the Freetown capital.
"You had to be a team player (but) the national staff were so grateful for the international help."
Upon arrival, patients were triaged into different tents, including "probable", "suspect", "confirmed" and "convalescence".
Confirmed cases were in the "red zone" where they were isolated and managed.
Nurses co-ordinated entries into the "red zone", which were strictly limited for safety reasons.
All staff had to wear personal protective equipment (PPE), with stints in the red zone limited to 30 minutes due to fainting, dehydration or exhaustion risks.
"With temperatures averaging 30 degrees Celsius, working in PPE was difficult. It was like being wrapped in cling wrap.
"Other factors I had to consider were the limited medical resources, the provision of patient care under strict isolation protocols, leading a large team of national staff and working in a politically fragile country."
Hygienists - called "donners" and "doffers" - also sprayed the staff with chlorine, which kills ebola, on every entry and exit in the red zone.
Ms Nash said time off was spent at a nearby beach, visiting cafes and shops and in their hotel.
But they had to avoid markets and crowded areas and wash their hands in chlorine and have their temperature taken every time they entered their hotel, cafes or supermarkets.
Ms Nash said cultural west African practices helped spread the ebola virus, particularly because poverty forced many to turn to traditional healers rather than proper medical care, and bodies are washed after they die.
"There were something like 365 cases of ebola related to the funeral of a traditional healer."
After Ms Nash returned to Australia, she spent three weeks in quarantine at her Newington home, taking her temperature daily without incident.
However, she said the thought of getting the virus was never far from her mind.
"I was constantly checking my gloves to make sure there were no cuts in them."
But she also said it was an experience she wouldn't have missed.
"On reflection, my advice to nurses working in primary care would be to never underestimate the diversity of your skills and knowledge.
"The most important aspect in taking on a new and challenging venture is adapting to the environment, conditions and possible lack of resources."
fiona.henderson@fairfaxmedia.com.au