When Lorraine Granger-Brown first heard she a had a small lump in her breast, she didn’t worry overly about it. Discovered during a routine mammogram in 2015, it was 1cm x 1cm – tiny, to her thinking. She had a core needle biopsy the same day, and the general opinion was that it was unlikely to be cancer.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading

The biopsy results were inconclusive. After discussing further treatment options in Ballarat and feeling unsure about what was proposed, Lorraine sought a second opinion. She went to the Peter McCallum Institute in Melbourne. Specialist breast surgeon and surgical oncologist Professor Bruce Mann was not concerned greatly by her case either. He felt on first appraisal it might be a ductal carcinoma in situ (DCIS), an abnormal cell growth in the milk duct of the breast. He booked Lorraine in for surgery in June 2015 at The Royal Melbourne.
The surgery revealed that although the tumour was small, it was Category-3 cancer, aggressive and malignant. Following a second surgery at the Peter Mac on June 30 to clear the margins of the removed tumour, and discussion at an inter-disciplinary meeting, there was an equal division amongst her treating doctors as to whether or not Lorraine, at 52, should undergo chemotherapy.
Chemotherapy. It’s a term that is not well-understood, emotive and frightening. A course of drugs designed to attack cancer cells and stop them from multiplying, its range of side-effects are feared – loss of energy, skin changes, anaemia, kidney damage, cognitive lethargy, hair loss.
Lorraine, on the advice of Professor Mann, decided to undertake a Oncotype DX Breast Cancer Assay.
While it is covered by health schemes overseas, the assay is not currently covered by Medicare in Australia, nor widely offered to women. It assesses a patient’s likelihood of suffering a recurring cancer, in order for them to make a choice about undergoing the rigours of chemotherapy. For Lorraine, whose background was in supplying medical equipment, the $4,500 cost of the assay she had to bear was justified against perhaps avoiding chemotherapy’s consequences.
Her result determined that she was in the high recurrent risk group. She chose to undergo the course of chemotherapy, as she says, for the right reasons. It wasn’t just a cautionary choice; it was necessary for her survival.
Lorraine Granger-Brown is a piano and singing teacher. She spends hours in close contact with her students each day. The thought of losing her hair was “not an option”. Her treating specialist in Ballarat, Professor George Kannourakis, said that her particular course of chemotherapy meant that her hair would be gone in two weeks.
“It was so important for me to try and have some semblance of normality, because I’m teaching young children. If I could make myself not look so different, not to frighten them.”
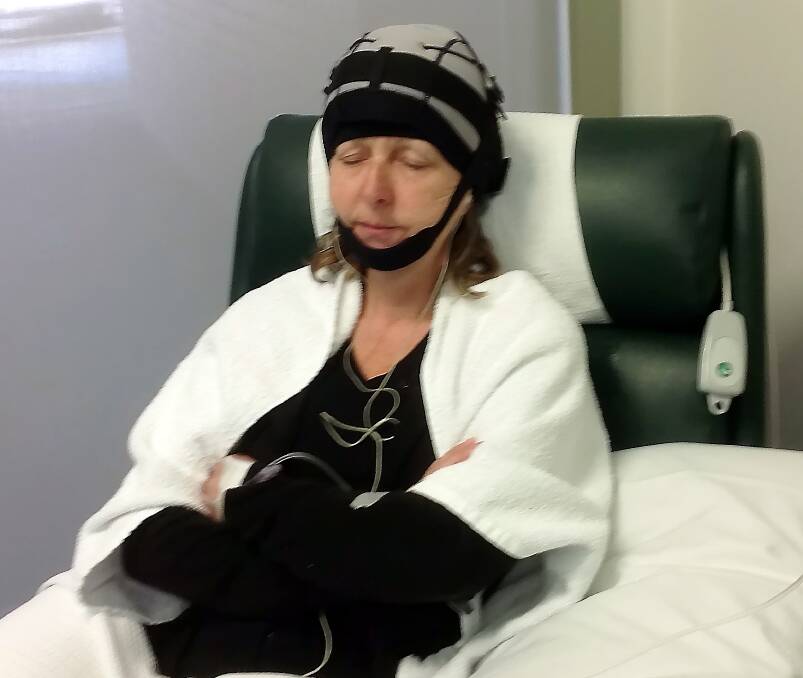
But the practice at which Lorraine was being treated, Ballarat Oncology and Haematology Services, offered a possible solution. The Paxman Orbis Scalp Cooling System is a bloodflow-inhibiting procedure designed to minimise hair loss during chemotherapy.
“Professor Kannourakis pointed out to me the cooling cap might be a great thing to try. The downside would be my chemotherapy, instead of taking about two and a half hours, might take six. Some women find it incredibly uncomfortable, it brings on a massive cold migraine because your head is frozen. And there's no guarantee of success.”
Kate Wyatt is the practice manager. She describes the procedure.
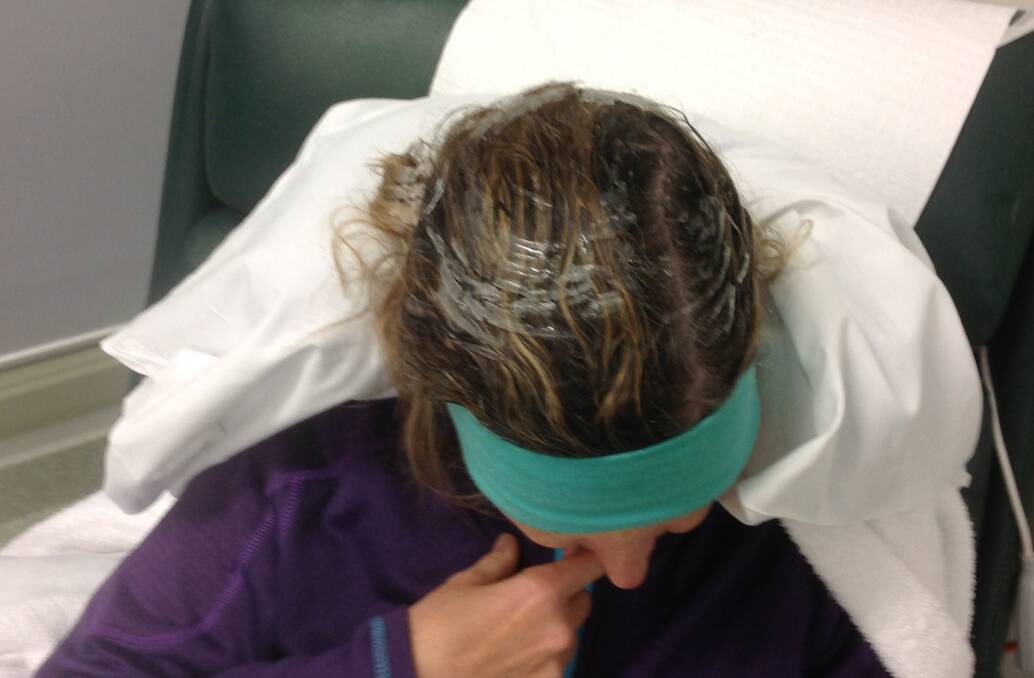
“It drops the scalp down to minus-four degrees Celsius. We wet the hair down with a moist conditioner, and fit a silicon cap over the head. It’s like a thick rubber cap with fluid running through it. It is in complete contact with the top of the head where the blood flows. It stops the blood flowing through the hair follicles.”
“We’ve had numerous women get fantastic results from it and retain their hair. Women who have had cancer in the past and lost their hair, and have had a cancer recurrence and used the scalp cooling, have kept their hair this time around.”
Ms Wyatt says the results can vary, with some women experiencing hair thinning, but that most women have retained their hair.
For Lorraine, it meant she was able to continue her teaching life with confidence.

“It wasn’t that bad. It’s not comfortable, but after the first ten minutes, if you’re listening to some beautiful Chopin or soothing music, you can just block it out.”
“I feel so sad that other women that I have met are so panicked about their cancer diagnosis that they rush into making their decisions – ‘It’s cancer, I better book in for surgery on Monday’ – instead of just taking that step back.
“I met a nurse in my radiotherapy session from Ballarat Base Hospital who couldn’t believe I’d undergone chemotherapy because I had all my hair, and she was bald.
“She said, ‘they told me it didn’t work’. Her belief as a nurse within the system was that it didn’t work.
The Paxman system is offered as a free adjunct to patients undergoing chemotherapy treatment at Ballarat Oncology and Haematology Services at present, but Lorraine Granger-Brown hopes to see it offered across Ballarat widely, to help alleviate at least some of the suffering that patients going through chemotherapy suffer.
“Chemo is like something I can’t describe. It’s the most… it’s just… I don’t know whether I would do it again. Maybe the first five to six days – you don’t feel like yourself, you feel like you’re walking in someone else’s skin. I felt like I was barely alive. Terrible bone pain, all through your jaw, all through your skull, all through your facial bones. And then after about day six you think ‘oh OK, I will go and have a cup of coffee, but you still feel weak.”

