
FRONTLINE Ballarat health workers are set to receive specialised skills training to manage ice users who are injecting the drug.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Not-for-profit health safety organisation Penington Institute will deliver the program in Ballarat on Wednesday in a bid to reduce the burden of ice-related issues in the community and build confidence in health workers meeting the problems firsthand.
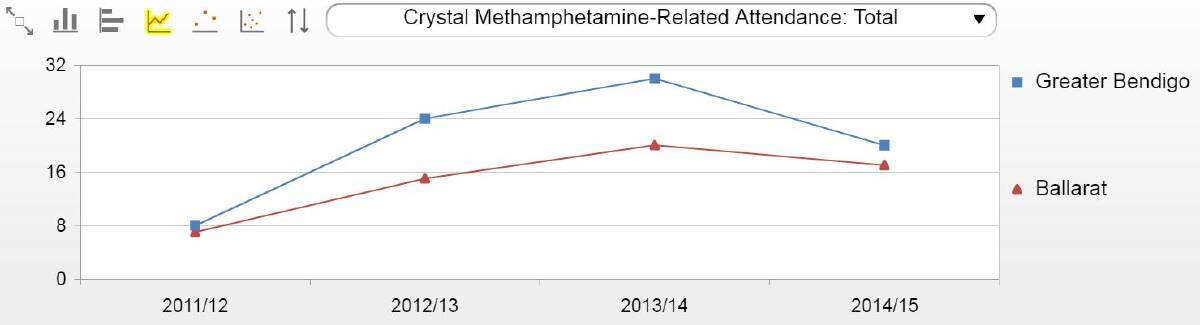
Ice-related ambulance attendances in regional Victoria have boomed from 94 to 467 in the three years to 2014/15, according to Ambulance Victoria drug and alcohol statistics.
There were 17 ice-related ambulance cases in Ballarat in 2014/15.
Penington Institute chief executive officer John Ryan said that while ice, the crystalline form of methamphetamine, was most commonly smoked there was a growing number of people injecting the drug and this had particular implications on mental and physical health.
“People who inject ice are at the more serious end of the drug use spectrum, and frontline workers face significant challenges when providing services to them,” Mr Ryan said.
“The education campaign, called Injecting ice in the Country – Healthier Approaches, covers themes identified by rural and regional frontline workers as areas they wanted to learn more about.”
Training will focus on developing practical strategies to meet the needs of clients.
This includes engaging clients in needle and syringe programs (also known as needle exchanges), safer injecting and harm reduction, ice use in the country, and physical and psychological impacts of ice use.
Videos present views of NSP and other health experts about how they manage issues in their workplaces, which could often serve up competing priorities.
There will also be a session to improve support and access to NSP services for Aboriginal people who are injecting the drug.
Ballarat Community Health harm minimisation coordinator Pauline Molloy said NSPs were an essential part of the health system.
“They are working on the front line serving a client group which can be quite marginalised,” Ms Molloy said.
For every dollar spent on NSPs, four dollars are saved in direct health care costs (like prevention of blood-borne viruses) and $27 is saved on cost to the community (including saved productivity for illness), according to Penington Institute.


