Margaret Daly still remembers the days she would visit her husband John at his nursing home, only to find him restrained in a chair with the straps so tight they almost cut into his genitals.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
She remembers, too, the evenings she would find him distressed in his darkened room, restrained to a wheelchair facing the corner.
She recalls, quite distinctly, the way staff would sometimes "put him in the corridor like a bad smell", leaving him to walk around aimlessly until he became agitated.
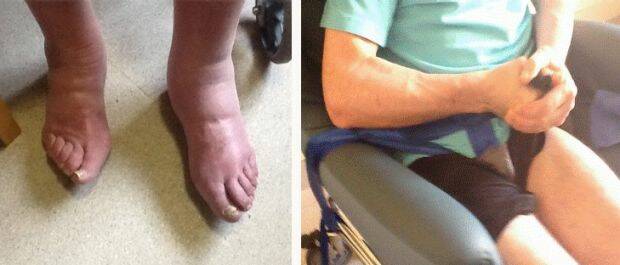
"Then they'd just tie him up in the chair again," she says. "He was restrained for so many months his genitals were red raw and his feet became swollen and blue. It was so dehumanising, like something you'd witness at Guantanamo Bay."

John Daly died in June 2014 - from respiratory failure and sepsis - about two years after he first arrived at the Allambee Nursing Home in the Melbourne suburb of Cheltenham where he'd been admitted with dementia, epilepsy and depression. He was 64.
But it has taken until now for Mrs Daly to speak out, convinced that the way he was treated not only hastened his death, but raises a pressing question of Australia's aged care system: where do you turn when things go wrong?
"It all boils down to the fact that there's no accountability in these homes," she says. "You can complain all you like, but it's rare that your concerns are taken seriously. Even when there's an investigation, it feels like a whitewash."
On paper, Allambee has all the hallmarks of a good nursing home: a 35-bed facility tucked away in Melbourne's south east, a 24/7 registered nurse, and full accreditation with the national Aged Care Quality Agency standards.
It has passed with flying colours all three of its federal audits over the past 10 years, meeting 44 out of 44 expected outcomes - from clinical care and staff development, to specialised nursing and complaints handling.
But Mrs Daly - along with others who spoke to Fairfax Media about their experiences at the home - remain unconvinced.
While physical restraint is supposed to be a last resort, Mrs Daly claims John spent four months strapped to a wheelchair without her consent, sometimes for up to 12 hours at a time. Sleep charts tracking his movements over a two-week period confirm that he rarely slept in a bed, which she says exacerbated his back problems and added to his psychological distress.
She'd beg staff not keep him tied up, but they would cite a range of reasons: that he didn't want to walk; that he was being aggressive; that it would minimise falls, or there weren't enough nurses to supervise him.
Eventually, Mrs Daly lodged a formal complaint with the Aged Care Complaints Scheme - the forerunner to the current scheme - on several grounds. John was being restrained for "excessive periods"; she was excluded from "meaningful input" into his care; he was not receiving adequate medication.
Yet while the scheme conceded that "staff did not follow their own [restraint] procedures", it was unable to determine whether the time John spent strapped to a chair was excessive. Eventually, it ended the inquiry "on the basis that the service provider had addressed it to my satisfaction". Most of the concerns Mrs Daly had raised were dismissed in a similar fashion.
"Since then, I've been to [the government's new, independent complaints body] the Aged Care [Complaints] Commissioner, I've been to the Victorian Ombudsman, I've been to [Victorian Senator] Mitch Fifield ... but because the [old] Aged Care Complaint Scheme has already looked into it, there's not much anyone else will do," she says.
Fairfax Media tried to contact staff at Allambee House, but was directed to Monash Health's public affairs unit. In a statement, a spokesman simply said, "Monash Health cannot comment on individual cases due to patient confidentiality".

Quality control?
Nursing homes must be accredited by the government to receive public funding - the vast bulk of their income. The accreditation system is the basis of the government's boast that Australia has a world-class aged care system.
Every three to five years the Aged Care Quality Agency audits a home and measures it against 44 "expected outcomes". There are also annual, unannounced visits.
Critics such as Lynda Saltarelli from community group Aged Care Crisis say the quality agency is not independent. It acts, she says, as a reserve bench for the nursing home industry. Critics also say the accreditation standards are far too broad and audits too shallow.
The 44 standards include "expected outcomes" such as that "care recipients receive appropriate clinical care"; "adequate nourishment and hydration" and that "challenging behaviours are managed effectively".
"They are so general in nature that anyone could pass," says Gary Morgan, a former auditor with a top-10 Australian company, whose wife lived in a nursing home that he says was driven by profit and not care.
"I'd throw every one of [the standards] out ??? they're subjective whereas they should be objective. It should be, 'All residents, especially in high care, should be fed their meals within 15 minutes of arrival in the dining hall'; 'All residents of high care should have continence pads changed every six hours'."
The government is conducting a review but new draft standards released this year suggest similarly subjective measures may take over.
The Quality Agency boasts that "more than 97 per cent of all residential aged care facilities that went through a full audit were assessed as meeting all expected outcomes". An agency spokeswoman said the high rate of compliance "demonstrates strong and sustained improvement in overall industry performance".
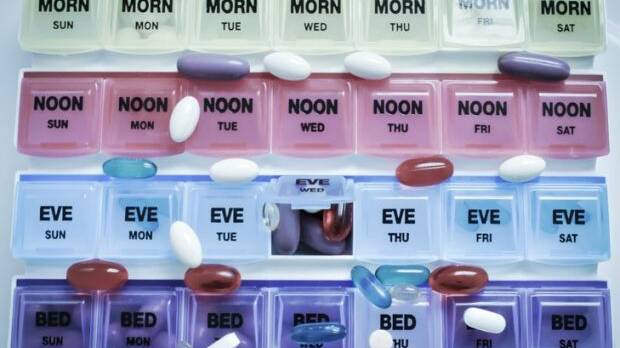
Biscuits, cheese and a jam roll
Nursing homes are given several months notice of an upcoming audit and the big providers have "accreditation teams" that sweep in to make sure their staff say the right things.
Helen Hardy's mother died in 2015 at an aged care home in Lakes Entrance, Victoria, run by for-profit company Opal Aged Care. June Johnston had been a mild-mannered woman until dementia took over, when, according to Helen, she became "very difficult".
In 2013, witnesses saw a carer at the home hitting June. The worker was charged with assault but the case was dismissed when she produced statutory declarations from co-workers saying she was hitting lice, or fleas, off Johnston's head.
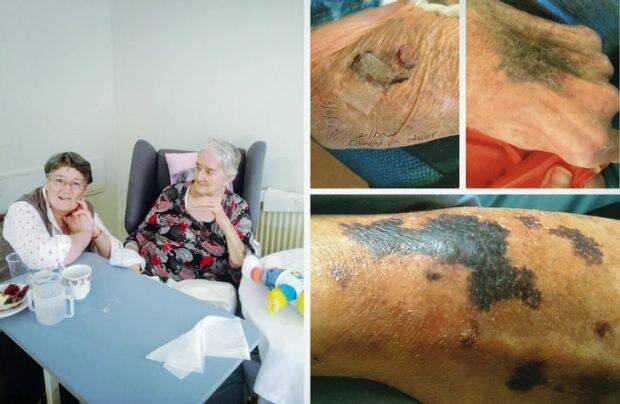
And then there were the bruises.
"We have no way of telling how she got these - but every day I'd find a bruise and they'd say, 'We don't know how it happened'. But they'd already have dressed it," Hardy said.
The home was "absolutely appalling," she told Fairfax Media, "except when accreditation was on and they wanted to put on a show".
"Then they have all the staff, all the residents up and clean and shiny, had bingo all day, extra diversionary staff, extra lifestyle staff, a pharmacist for three months beforehand.
"They repainted everything, put up a false menu, biscuits and cheese, and jam roll. Jam roll! I kept thinking, 'They won't pass this'. Then they ended up getting 44 out of 44.
In response to questions, Opal released a statement saying, it "takes its responsibility to staff, residents, and families seriously" and its commitment to "meeting our high standards, and the expectations of those we care for, is unwavering".
On the bruising, it said, "we do not, and will not, tolerate behaviour that doesn't align with our values or that puts the safety of residents and/or staff at risk".
Since a number of reports on ABC's 7.30 about Lakeview, it has been through a three-day unannounced visit from the accreditation agency, and passed all 44 standards.
"I worked for an organisation which was told accreditation was due in three months, and it was a mad-house," says another private sector whistleblower.
"We were supposed to have Occupational Health and Safety on the monthly meeting agenda, and this place hadn't done that for more than three years. So I had to go back to all the old meeting agendas, add OH and S to them, and then reprint them."
Dr Michael Wynne, from Aged Care Crisis, says accreditation is not working: figures from the Department of Health acknowledge that between 26 per cent and 42 per cent of residents in Australian nursing homes have pressure sores. In the US, it's 6.2 per cent.

When things go wrong
When something goes wrong in a nursing home, the burden falls on sometimes bereaved and traumatised family members to take on the home. Former nurse and Charles Sturt University academic Associate Professor Maree Bernoth says many people are frightened to make a complaint.
Partly it's a generational issue: people born in the 1930s and '40s are more likely to accept authority without questioning it. But in some cases, families fear their loved one will be punished for speaking up.
Even so, Aged Care Complaints Commissioner Rae Lamb received 4713 complaints about nursing homes in the last financial year.
Complaints reports are not made public and the commissioner is prevented by legislation and the Privacy Act from naming and shaming homes. Lamb says if that were to change it would be up to the government, adding, "It's clear the public wants more transparency around this information".
If wrongdoing is found, Lamb says she tries to make sure homes change their practices. The bulk of complaints are "resolved within 30 days", and about half "to the satisfaction of the complainant," she says.
Kaye Weston is not satisfied. She believes her mother's death from a pair of gangrenous pressure sores in a not-for-profit home, Chamberlain Gardens, last year should have been an objective indicator that the care was not up to scratch.
So she complained to Ms Lamb's organisation. Its report laid out in detail what had gone wrong. The home published nothing and continued accepting residents.
Six months after Dawn Weston's horrifying death, Chamberlain Gardens on the NSW Central Coast was audited. The report, which appears on the Quality Agency website, appears to refer to Dawn's death like this: "In April 2016, feedback from a care recipient's representative identified the need to improve the management of complex wounds".
Among the changes were a "closer monitoring role" for the home's care manager, and putting registered nurses (rather than care assistants) in sole charge of wound care.
Weston asks: "What's the point of changing their procedures if they already weren't following the procedures they had?"
Ross Peden, chief executive of Christadelphian Aged Care, which runs Chamberlain Gardens, said the home had "addressed the relevant issues to the satisfaction of the Commissioner".
The accreditation audit resulted in the home being successfully reaccredited, meeting all 44 standards. It can now operate without another major audit until 2020.
Weston is now arguing the case before the nurses' professional regulatory body. That process continues.
'Difficult' families
Sometimes the decline of people in nursing homes becomes the scene of serious conflict between the home and family members.
Dealing with Difficult Families was the title of a speech presented at an aged care industry conference last year by lawyer Arthur Koumoukelis.
As his audience of aged care providers took notes, Koumoukelis spelt out the ways in which things could go wrong from the point of view of the home - family members abusing their relative emotionally, physically or financially.
"Aged care facilities face complex and challenging family situations daily," Mr Koumoukelis told Fairfax Media. "This requires a number of methods to ensure that their residents' interests, safety and rights are protected."
If the dispute could not be resolved by normal means, he told the audience the home had the right to play tough: bringing in an "unfriendly third party", a ??"bad cop??", or sending a "lawyer letter".
If the complainant persisted, the home could "exercise rights as owner of premises - refuse entry to people who create a nuisance or disrupt your business".
Lee Annear was banned by her mother's for-profit home in Western Australia after a dispute with her own siblings and an adverse finding from the public advocate. The dispute arose over her desire to feed her mother.
As her mother died, Annear stood vigil with a security guard at her side.
A change in the wind?
A series of inquiries, including one by the federal government, into the Oakden home in South Australia is looking into both the accreditation and complaints systems after a decade of mistreatment and mis-medication of residents at the home, as well as a sexual assault by a carer and a murder by a resident.
For most of that period, Oakden, a state government-owned facility, passed its federal accreditation audits.
"The review that will come out of Oakden will certainly be a potential pointer to what we need to seriously consider," Aged Care Minister Ken Wyatt told Fairfax Media.
Confronted with complaints, he said, some homes "have just pulled down the shutters and not dealt with it; that's when people get angry and they become frustrated".
He was also "very conscious" that the complaints system lacks teeth, and "we have to be serious about what sanctions do apply."
Wyatt also acknowledges that the Australian system lacks transparency. Unlike in the US, where a nursing home's failings, complaints and negative findings are published and searchable online, Australian consumers must rely on advertising and bureaucratic government reporting.
At the time of writing, the government's "Current Sanctions" web page for nursing homes offers nothing on any state or territory except Western Australia, where there are some scant details on Morrison Lodge.
Cameron O'Reilly, whose Aged Care Guild represents the nine largest for-profit nursing home companies, said social media and the higher expectations of the baby boomer generation meant there was "more opportunity now with residents and consumers to expose where there have been failings.
"There will be more expectation on industry to be transparent in future."
But industry lobby group Leading Age Services Australia warned any more transparent complaints mechanism should give the nursing home a right of reply, as well as identifying what proportion of complaints are "vexatious". It said the quality of the Australian industry was high by world standards, but was threatened by a few "bad apples".
Aged care law specialist Rodney Lewis wants to see a compulsory arbitration clause in every residential care contract.
And aged care expert and Monash University professor Joe Ibrahim foresees a time when a big law firm takes on some cases.
"So potentially you'd end up with Slater and Gordon, pro bono, taking on a case of false imprisonment for a number of cases for a nursing home listed on the stock market, so you have a law firm worth billions fighting listed aged care worth billions fighting out on human rights.

