A perfect storm of factors is forcing unprecedented demand on the Ballarat Base Hospital emergency department.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
GP shortages, a growing population, regional demand and unnecessary presentations are combining to put added pressure on resources in recent months.
During that time The Courier has been inundated with stories of long wait times, patients being sent elsewhere and even leaving unseen.
The question remains whether existing resources at Ballarat Health Services can cope with demand and whether the increasing pressure is affecting health outcomes.
A shortage of general practitioners is increasing the demand on the Ballarat Base Hospital emergency department.
Patients who cannot secure a same day appointment for urgent matters with their regular GP are being told to visit walk-in clinics where they can face up to three hour long waits.
Some have reported being told by receptionists to go to the emergency department instead.
A lot needs to change with health services.
Medical professionals and patients have called for more general practitioners and a second major walk-in clinic to help meet the demand in Ballarat.
A medical professional told The Courier in January up to 200 people a day were being turned away from a walk-in clinic, with patients left with nowhere to turn but the emergency department for urgent medical help.
On Thursday they said the situation at the medical clinic had improved, with more doctors on staff and nearly all patients presenting now being seen.
But the pressure on general practitioners remains high, with around 30 people queued outside Eureka Medical and Dental Centre before it opens at 7am each morning.

A patient who asked to remain anonymous was part of the queue on Thursday morning and said they waited two hours to be seen after the doors opened.
“Ballarat needs another walk-in clinic like Eureka and another public hospital. The services we have are just not coping,” they said.
One medical professional said the pressure on the doctors at Eureka Medical Centre was immense.
“They must feel anxiety when they rock up to work and see that many people waiting to see them,” they said.
“Everyone is trying to do their best. It is just the number of people the lack of infrastructure and health workers is not equipped for.”

Eureka Medical and Dental Centre did not comment.
A Department of Health spokesperson told The Courier the Rural Workforce Agency Victoria was completing an annual Health Workforce Needs Assessment in Ballarat.
The agency will provide details of the assessment to the department in the first quarter of 2019.
“Under the District of Workforce Shortage System, Ballarat is considered to be a non-District of Workforce Shortage area as the general practitioner to population ratio is better than the Australian average,” the spokesperson said.
“Consequently, residents of Ballarat enjoy better access to general practitioner services than the Australian average. The annual Health Workforce Needs Assessment process completed by the Rural Workforce Agency Victoria takes into consideration factors impacting on the health workforce such as health care demand.”
The pressure on services in Ballarat is amplified by residents travelling into the city for health care from surrounding small towns where general practitioner numbers are low.
A letter from Dr Michael Connellan from the Ararat Medical Centre said the centre was currently operating with five doctors less than the same time last year.
“In recent weeks it has been very apparent that we do not have enough doctors in Ararat to service the needs of the community," he said.
"People have been unable to get an appointment with their usual GP, and in fact have been unable to get a timely appointment with any GP for ongoing management of their health needs.”
“The recruitment of doctors to rural towns remains an ongoing difficulty - not just in Ararat but throughout Victoria.
“We are looking forward to welcoming some new doctors in the next few months depending on approval from Australian Health Practitioner Regulatory Agency.”
UFS Pharmacy chief executive Lynne McClennan said difficulties employing suitably trained and experienced general practitioners continued while Ballarat was not a designated workforce shortage area.
“Even when it is designated a workforce shortage area - meaning we can recruit a general practitioner from overseas - it is still very very difficult,” she said.
Ms McLennan said patients had options other than the emergency department if they could not see a general practitioner.
“Patients can be seen by the nursing service at the UFS Pharmacy on Sturt Street for minor health concerns,” she said.
“There is also the 24 hour pharmacy service that can give advice. Often patients can come into the pharmacy overnight and may be told to go to emergency, but there would be some patients who go straight to emergency when they possibly could have seen the pharmacist.”
Australian Institute of Health and Welfare data shows the number of people presenting to the Ballarat Base Hospital emergency department increased 8.4 per cent in the past year.
Almost 60,000 people presented to the emergency department in the 2017-2018 financial year, compared with 54,704 the year before.
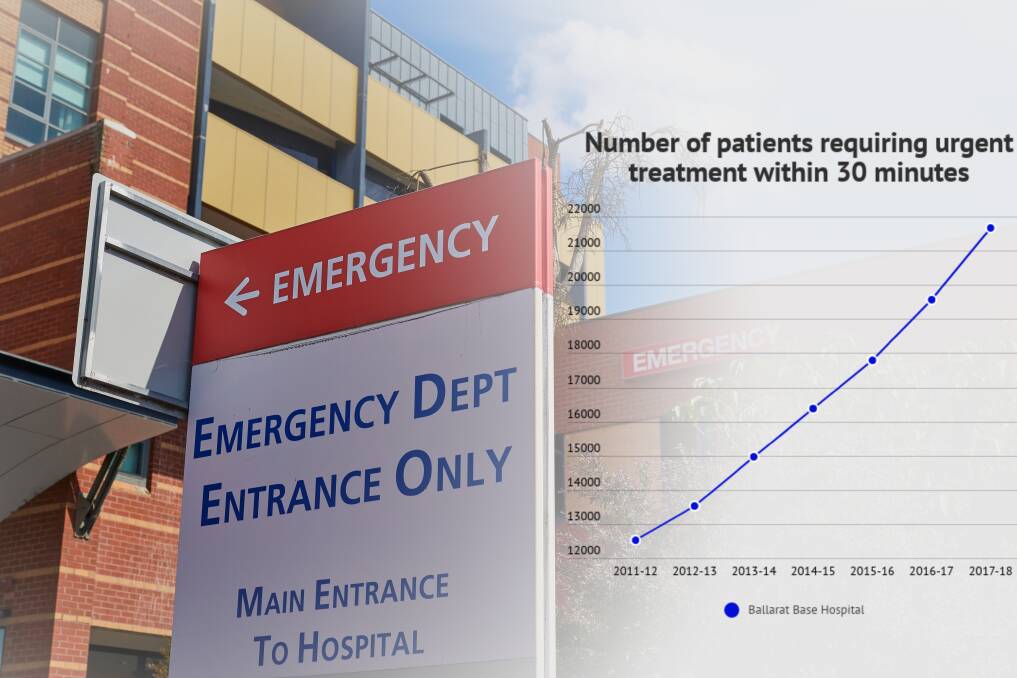
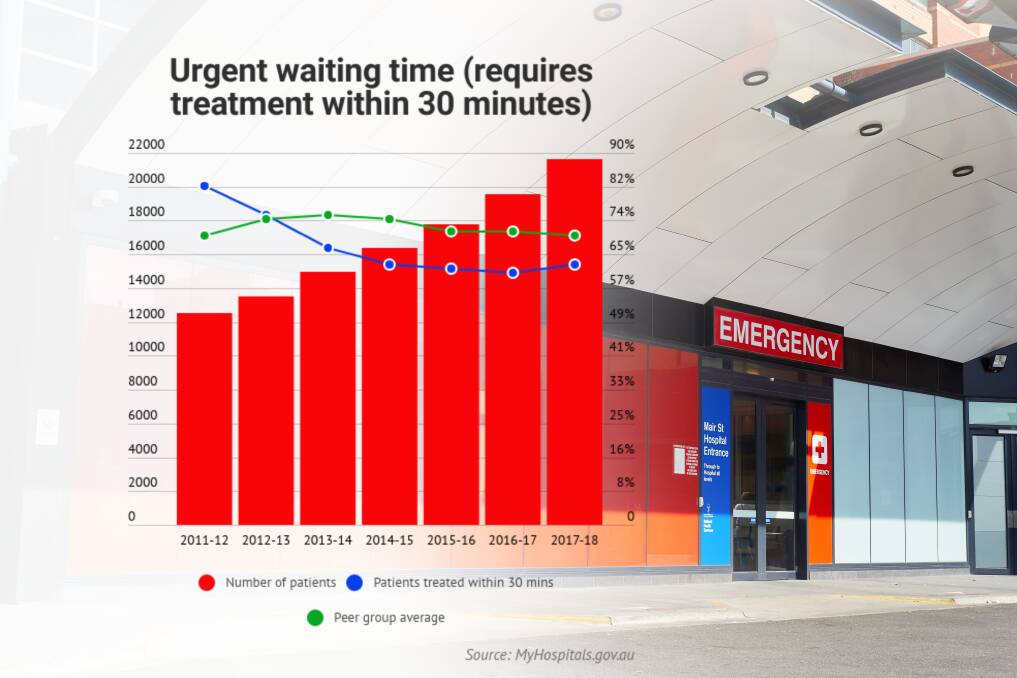
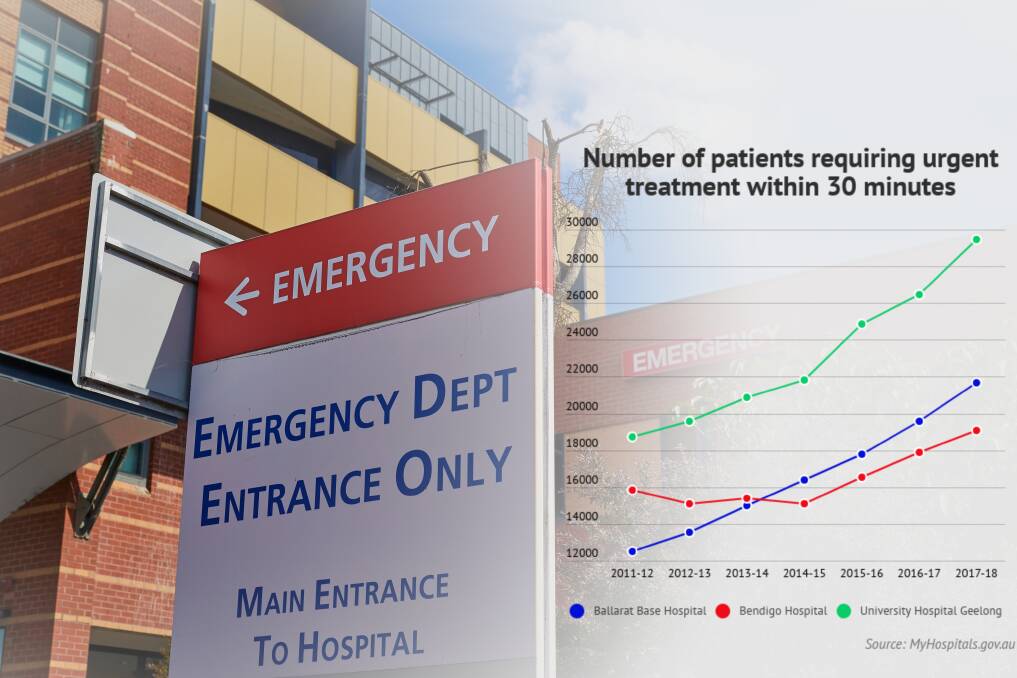
The number of patients requiring urgent treatment within 30 minutes increased by more than 2000 in 2017-18 from the previous year, while the number of patients requiring semi-urgent treatment increased by more than 1500.
The data shows Ballarat Health Services was below peer group average for patients treated within appropriate waiting time for all categories other than resuscitation (all patients resuscitation patients were treated within two minutes of arrival).
Ballarat Health Services executive director acute operations Ben Kelly said the hospital ‘occasionally’ experienced days in the emergency department where there was an increase in demand.
“On these days we work across the whole of Ballarat Health Services to put in place systems and measures to cope with this demand. This includes assessing all available beds across our Base Hospital and Queen Elizabeth Centre and moving patients to the most appropriate spaces to receive care, which includes our mental health services and facilities,” he said.
“We continue to display our waiting times in the emergency department for those community members who do come in and offer access to general practice surgeries via a dedicated phone in the waiting room.
“We will always treat the most urgent illnesses and accidents first and appreciate the patience and support of our community during these times.
“Work continues on the planning of the redevelopment of the Base Hospital and we maintain our commitment to engaging with the community during this process.”
A Victorian government spokesperson said the funding for Ballarat Health Services has increased by $72.84 million, or 32.4 per cent, since 2014/15.
“We know at times of peak demand there is pressure on Ballarat Base Hospital – that’s exactly why we’re building a bigger, better one,” the spokesperson said.
“Our $461.6 million Ballarat Base Hospital rebuild will enable hard-working doctors and nurses to treat more locals, in the best facilities.”
One Ballarat resident said she lodged a formal complaint to Ballarat Health Services after her mother was told to go home from the emergency department without seeing a doctor.
Her 68-year-old mother had fallen at home, been transported to the emergency department by ambulance and placed in a wheelchair in the waiting room around 1.30am.
The daughter said her mother waited in a wheelchair for more than two hours and was told she would not be seeing a doctor and would be discharged.
“There was no doctor seeing her, no x-rays taken, no ultrasounds done. All I got told was to give the radiology department a call to take mum in to them,” she said.
“Mum felt like she was abandoned and lost. There was no one around if she had a problem, and no one was there to listen to her. I only saw four staff members, two at the front desk, two nurses and a cleaner.
“She was technically discharged without the clearance of a doctor. I’m no medical professional but to me that seems very unethical.
“When I rang to speak to the radiology department I couldn’t get in until eight days later.
“A lot needs to change with health services. They need more doctors on during non-peak times. My mum was there for a good three hours and didn’t even see a doctor.
“The government needs to start stepping in and looking at emergency departments especially in regional area.”
The resident told The Courier Ballarat Health Services had contacted her saying they were were working through her complaint.
"He fell like a bag of spuds": father's anger at son's treatment
When Gavin Boyce suffered a petit mal epileptic seizure on Australia Day this year, his father Ken didn't have any idea of the hours of pain his son was about to endure.

Gavin suffered the attack while walking down the stairs in his family home in Creswick, and in falling twisted his ankle so badly that his ligaments and tendons were torn.
"At 6 o'clock he was at home and he went to walk down the back to go to the toilet," former dairy worker Ken Boyce says.
"We've got three steps in the middle of the house, and he had a petit mal at the top step and he took one big step to the bottom, and his foot hit the side of the step; he went right over on it and it took his full weight, and he fell like a bag of spuds.
"When I got down there his ankle wasn't pointing in the right way at all; I had to straighten him out because I thought he was going into a proper fit. But he didn't, thank Christ."
Gavin Boyce suffered a brain injury at 18 months after his anterior fontanelle fused prematurely (craniosynostosis), causing pressure within his skull and requiring major surgery. His father says his brain literally 'had nowhere to go, his head refused to grow.' He suffers epileptic seizures as a result of the injury.
Seeing his son's ankle turn black and swell instantaneously, Ken Boyce assumed it was broken and called an ambulance, which was dispatched from Ballarat and arrived in 25 minutes.

Mr Boyce said his son was extremely distressed.
"With his brain injury, anything like that really freaks him out. He thought he'd broken his ankle, and I wish he had, actually, because it would have healed quicker."
The ambulance medics told Mr Boyce his was their first call, giving Gavin the chance to get to Ballarat Base Hospital quickly before they were called in to the system, which was receiving large numbers of requests for urgent treatment at the Rainbow Serpent Festival being held that weekend.
Ken Boyce's 86-year-old mother-in-law travelled with Gavin in the ambulance, as his wife is confined to bed on a life-support machine with terminal cancer and could not be left unattended. Already being given morphine patches for her own rheumatoid arthritis which had moved into her spine, she decided the journey would be bearable.
"On the way in there, they got a call over the radio that the Base Hospital was not accepting any patients because of what was happening with all the overdoses at the festival, and they were just diverting everybody," Mr Boyce says.
Creswick just needs a small emergency department.
- Ken Boyce
He says he received a telephone call from his mother-in-law asking him if they could agree to being diverted to St John of God Hospital.
"I said 'whatever gets him fixed up'," Mr Boyce recalls.
"It was $190 in there (to St John of God) because he didn't get admitted, to see them and get a prognosis; and then we got a bill in the mail a few days later from Lake Imaging for $189 for an after-hours x-ray and report. So that's nearly $400 out of pocket."
After two hours treatment Gavin and his grandmother caught a taxi home to Creswick.
Mr Boyce said the treatment Gavin received at St John's was 'brilliant'; he simply didn't know what the costs would be. He says he's not disputing the amounts charged, although he would have liked to be advised of a prospective cost beforehand if it were possible.
He's more upset by the incapability of the Base Hospital to provide treatment on a weekend where, he argues, BHS management should have been better prepared for large numbers of cases presenting for treatment, including drug overdoses.
Mr Boyce said another woman came into St John of God at the same time Gavin was admitted after being being turned away from Ballarat Base emergency as well, after her son had suffered a similar injury in a motorcycle fall.
"She couldn't afford to pay, so she disappeared somewhere else, maybe Maryborough," Mr Boyce said.
"Ballarat's population is growing so quick, but nothing else is. You've got a brilliant little hospital at Creswick; my wife refuses to go to the Base, because she's had so many bad experiences stuck there for hours and hours and hours in pain. It (Creswick) just needs a small emergency department."
Gavin Boyce faces at least six more weeks on crutches and further treatment.
Have you signed up to The Courier's variety of news emails? You can register below and make sure you are up to date with everything that's happening in Ballarat.

