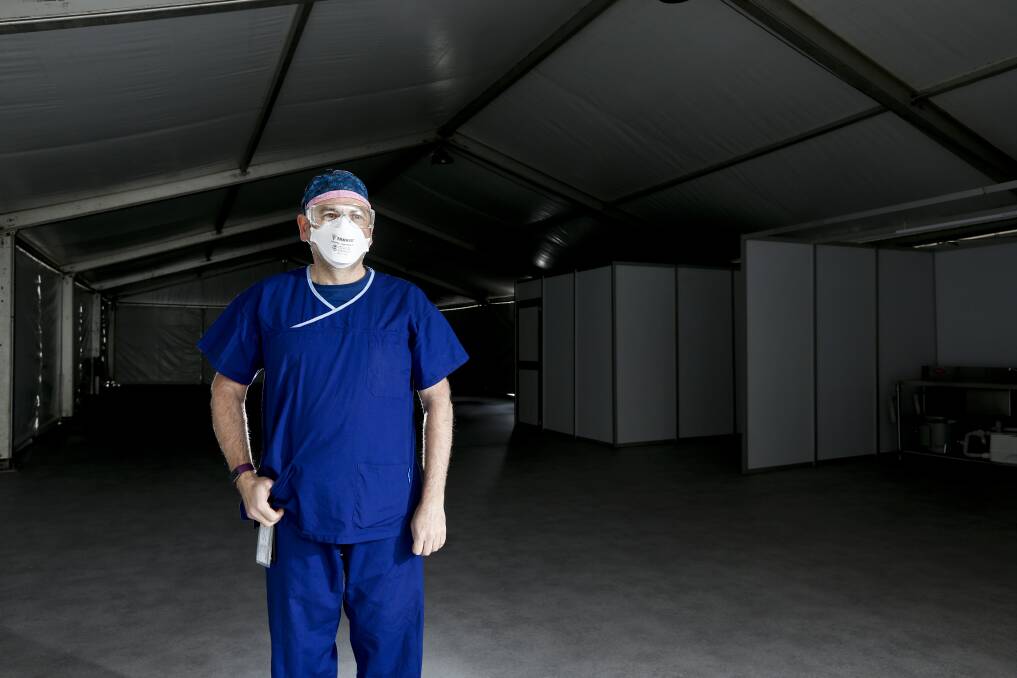
NURSE Marcus Hovey's message to the Ballarat community is blunt: "stay off my ward".
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
That ward is now a COVID red zone.
Ballarat Health Services Base Hospital ward 2GP is now open to take adult COVID patients from across the state and while priority will be given to those in need across the Grampians region, Mr Hovey would prefer people get fully vaccinated and not be sick enough to need him team at all.
"But if you do come we're going to look after you. COVID disease is another respiratory illness, that's how we're managing it," Mr Hovey said.
"My team has been upskilled in the management of COVID. People have come in, they might be young but they compensate and compensate - they're talking and fine and all of a sudden they crash.
"It's about putting in the learning and nursing care for that and identifying early and getting our lovely intensive care liaison nurses to come in and work with us and the patients on the ward. They might go to ICU [intensive care unit], they might come back and stay with us, it just depends on the person."
People have come in, they might be young but they compensate and compensate - they're talking and fine and all of a sudden they crash.
- Marcus Hovey, COVID ward nurse unit manager
Ballarat's COVID team has been preparing and ready to face the largely unknown for 20 months now. COVID cases have come and gone but the team was preparing for an influx now the Base had become a streaming hospital.
There is still no certainty for what might be to come, given soaring case numbers across a state about to open up and the race to vaccinate still a big issue.
Mr Hovey said the situation and care guidelines were constantly changing. While this was a big challenge, he said communication with patients and staff was the key to staying ahead and feeling confident.
Patient access to technology was improving to touch base with loved ones and specialists. But Mr Hovey said it was a real lonely time for patients on the COVID ward. His team could not properly offer emotional support - but they tried.
RELATED NEWS
Shifts were undeniably tough for staff on the COVID ward too.
Staff were often in full personal protective equipment for eight to 12 hours a day. Mr Hovey has been ruling out double-shifts, instead adding a couple hours to shifts when needed and relying on surplus COVID-trained nursing staff to keep the ward safe.
Tea-breaks in an isolated tea-room, also for the ward's cleaning staff, are factored in more often to shifts - even just to allow staff the chance for a drink and toilet break. These were simple things Mr Hovey said people took for granted until they could no longer do so in full PPE.
Mr Hovey encourages his team to take annual leave and personal days to ensure they were 100 per cent on their game and refreshed for the ward's demanding needs. Just spending prolonged time out of full PPE could make a big positive difference, Mr Hovey said.
[Staff are] quite resilient. They keep coming to work, which is a good sign...It's really tough.
- Marcus Hovey, COVID ward nurse unit manager
"They're quite resilient. They keep coming to work, which is a good sign," Mr Hovey said. "...It's really tough. A lot of people are a little bit triggered too, 'oh, I've got to wear this again', but we get through that as well."
Ballarat's COVID ward is only set up for adult patients but Mr Hovey said it was possible older teenagers might be able to access care.
BHS' children's ward has processes in place for COVID care. Children in need are still sent to Royal Children's Hospital should they need hospital care for COVID.
BHS has also looked to Shepparton where there was some hospital care for COVID-positive children to consider how this might work in Ballarat if needed.
If you are seeing this message you are a loyal digital subscriber to The Courier, as we made this story available only to subscribers. Thank you very much for your support and allowing us to continue telling Ballarat's story. We appreciate your support of journalism in our great city.


