
A report published by scientists and disease experts at the Imperial College in London has prompted a lot of discussion among politicians as well as the wider population about how to tackle coronavirus.
Subscribe now for unlimited access.
or signup to continue reading
Its title may sound drily academic but the report, "Impact of non-pharmaceutical interventions (NPIs) to reduce COVID-19 mortality and healthcare demand", makes for compelling and sobering reading.
The Washington Post described it as "a chilling scientific paper" which "helped upend US and UK coronavirus strategies".
Here, The Courier outlines the main talking points, findings and suggestions.
Please note that this is intended as a snapshot summary only, and to understand the full nuances of the report, we strongly suggest you read it in full.
What's the report about?
The report is, in essence, an analysis of two separate strategies - using so-called non pharmaceutical interventions (ie no drugs) - to tackle the spread of the virus. It models which method would be the most effective - looking specifically at the US and the UK - and save the most lives, as well as the feasibility.
In a frank summary, its authors describe the global impact of COVID-19 as profound.
"The public health threat it represents is the most serious seen in a respiratory virus since the 1918 H1N1 influenza pandemic," outlines the report.
Referencing the absence of any current vaccine, it outlines two main strategies using so-called "non-pharmaceutical interventions" that can be used to reduce contact rates and slow the spread of the virus.
The first is mitigation, which it describes as "slowing but not necessarily stopping epidemic spread".
The second is suppression, which it defines as aiming "to reverse epidemic growth, reducing case numbers to low levels and maintaining that situation indefinitely."
China and South Korea are among the countries that have put this type of strategy in place. This would be a much wider and restrictive way of controlling and minimising the spread of COVID-19.
What does the report recommend?
While the authors recognise that mitigation will slow the rate of transmission and prevent a large number of deaths, they conclude that suppression is more likely ultimately to save more lives.
A mitigation policy - shorter term and less restrictive - is likely to overwhelm hospital beds, it says.
While the report deals with the scenario in the US and the UK - and stresses that the situation will be different for each country, and even regionally within countries - it says its findings are broadly applicable across high-income countries.
Here is the report's conclusion:
"Mitigation will never be able to completely protect those at risk from severe disease or death and the resulting mortality may therefore still be high.
"We find that optimal mitigation policies (combining home isolation of suspect cases, home quarantine of those living in the same household as suspect cases, and social distancing of the elderly and others at most risk of severe disease) might reduce peak healthcare demand by 2/3 and deaths by half.
"However, the resulting mitigated epidemic would still likely result in hundreds of thousands of deaths and health systems (most notably intensive care units) being overwhelmed many times over. For countries able to achieve it, this leaves suppression as the preferred policy option."
What would a suppression strategy involve?
In a nutshell, it would profoundly affect absolutely everyone in their daily lives - most likely for several months. Most people are already feeling the impact of the virus in one way or another, even if the number of cases remains at a relatively low level in Australia for now. Suppression would take things to a whole different level, and would involve the entire population "social distancing".
At the heart of the discussion is the rate of infection, defined as the basic reproduction number by epidemiologists.
By introducing suppression, the strategy would aim to push that right down and in effect put a lid on the outbreak.
Here is what the report says:
"A combination of case isolation, social distancing of the entire population and either household quarantine or school and university closure are required. Measures are assumed to be in place for a 5-month duration.
"Not accounting for the potential adverse effect on [emergency bed] capacity due to absenteeism, school and university closure is predicted to be more effective in achieving suppression household quarantine. All four interventions combined are predicted to have the largest effect on transmission.
"Such an intensive policy is predicted to result in a reduction in critical care requirements from a peak approximately three weeks after the interventions are introduced and a decline thereafter while the intervention policies remain in place."
Confirmed tests in Australia:
What's the catch?
There is one obvious challenge: could the population do this? This strategy is fraught with challenges not seen before by any current Western government. The essential caveat in the report is this: what works in one country may not work in others. Could the population of Australia behave the same as the residents of China?
Here is how the report puts that challenge:
"Suppression will require the layering of more intensive and socially disruptive measures than mitigation.
"The choice of interventions ultimately depends on the relative feasibility of their implementation and their likely effectiveness in different social contexts."
While the report concentrates on the feasibility of the strategies, it also alludes to other potential impacts on society too.
Again, in the authors' words: "Suppression, while successful to date in China and South Korea, carries with it enormous social and economic costs which may themselves have significant impact on health and well-being in the short and longer-term.
Another danger is that when a widespread suppression strategy is lifted, the epidemic would simply be delayed and infections would pick up from there.
From the report: "If intensive... packages aimed at suppression are not maintained, our analysis suggests that transmission will rapidly rebound, potentially producing an epidemic comparable in scale to what would have been seen had no interventions been adopted."
So how long would a suppression strategy be necessary?
The authors say the key to this is the discovery of a vaccine which could be used to immunise the population on a wide scale. This, they say, would stretch deep into 2021, or potentially even longer.
To avoid a rebound in transmission, these policies will need to be maintained until large stocks of vaccine are available to immunise the population - which could be 18 months or more
Here is what they say:
"Overall, our results suggest that population-wide social distancing applied to the population as a whole would have the largest impact; and in combination with other interventions - notably home isolation of cases and school and university closure - has the potential to suppress transmission....
"A minimum policy for effective suppression is therefore population-wide social distancing combined with home isolation of cases and school and university closure.
"To avoid a rebound in transmission, these policies will need to be maintained until large stocks of vaccine are available to immunise the population - which could be 18 months or more."
Would suppression tactics need to be in place all the time?
Not according to the report. Its authors say the idea would be to introduce those measures only when emergency hospital beds are about to run out.
We show that intermittent social distancing - triggered by trends in disease surveillance - may allow interventions to be relaxed temporarily in relative short time windows, but measures will need to be reintroduced if or when case numbers rebound
There would be a "trigger" point of new cases when measures would be re-introduced, thus slowing the rate of infection and giving hospitals more breathing space.
In the authors' words: "We show that intermittent social distancing - triggered by trends in disease surveillance - may allow interventions to be relaxed temporarily in relative short time windows, but measures will need to be reintroduced if or when case numbers rebound."
One of the key parts of the report is its modelling on the impact of measures introduced. These detail the likely pressures on emergency beds - and the number of deaths - according to a range of different scenarios, including the rate of infection and the stringency of measures introduced.
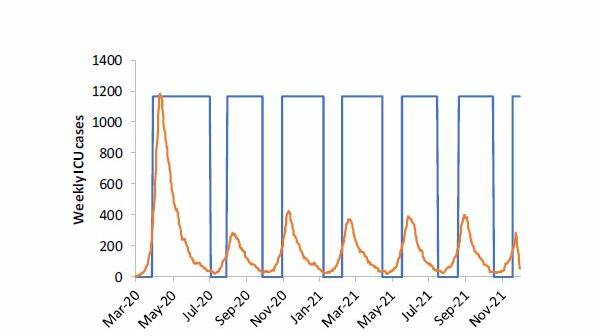
The report suggests "the proportion of time these measures are in force is reduced for more effective interventions". They would also be cut if the disease proves less infectious than feared.
Its authors warn that measures "would need to be in force for the majority of the two years" if its modelling is accurate.
What does this mean for Australia?
While the report highlights the cases of the US and the UK, its authors say the findings "are equally applicable to most high-income countries."
The number of emergency beds in Australia and the UK is roughly comparable (there are roughly 2,000 in Australia compared to around 5,000 in the UK, while the two countries populations are around 24 million (Australia) compared to 66 million (UK)).
The report says: "We conclude that epidemic suppression is the only viable strategy at the current time. The social and economic effects of the measures which are needed to achieve this policy goal will be profound.
"Many countries have adopted such measures already, but even those countries at an earlier stage of their epidemic (such as the UK) will need to do so imminently."
How confident are the authors that a suppression strategy would work?
The authors frequently refer to how understanding of the COVID-19 virus and the way it behaves is still in its very early stages. In its summary, it describes it as "a newly emergent virus", and that " much remains to be understood about its transmission."
They are understandably careful in drawing any cast-iron predictions or conclusions from their study, which they say has informed policymaking in the UK and other countries in the last weeks.
Here is the report's equivocal final paragraph, outlining the challenges ahead:
"However, we emphasise that is not at all certain that suppression will succeed long term; no public health intervention with such disruptive effects on society has been previously attempted for such a long duration of time. How populations and societies will respond remains unclear."
Who wrote the report?
The report was written on behalf of the Imperial College COVID-19 Response Team. Four organisations are cited as collaborators.
WHO Collaborating Centre for Infectious Disease Modelling
MRC Centre for Global Infectious Disease Analysis
Abdul Latif Jameel Institute for Disease and Emergency Analytics
Imperial College London
The lead scientist is Professor Neil Ferguson, who is the head of the MRC Centre for Global Infectious Disease Analysis team, as well as the director of the Abdul Latif Jameel Institute for Disease and Emergency Analytics.
To read the full report, see below:
RELATED STORIES
This article was published as part of our ongoing coverage about the coronavirus. We have removed our paywall from our stories about COVID-19. This is a rapidly changing situation and we aim to make sure our readers are as informed as possible. If you would like to support our journalists you can subscribe here.
Have you signed up to The Courier's daily newsletter and breaking news emails? You can register below and make sure you are up to date with everything that's happening in Ballarat.













